Orthomolecular Treatment of Mood and Behavior Disorders
Back to school routines are important and we want our kids to have the tools to face the school year with confidence and esteem. Nutrient or physiological imbalances make it difficult for kids to succeed and realize their potential. What we don’t want is our kids struggling with nutrient or physiological imbalances that we can do something about before they advance. The aim of this series is to increase parent awareness of commonly seen kid-specific nutrient and physiological imbalances and, to empower parents with insights on those orthomolecular (nutritional medicine) conditions that we can do something about.
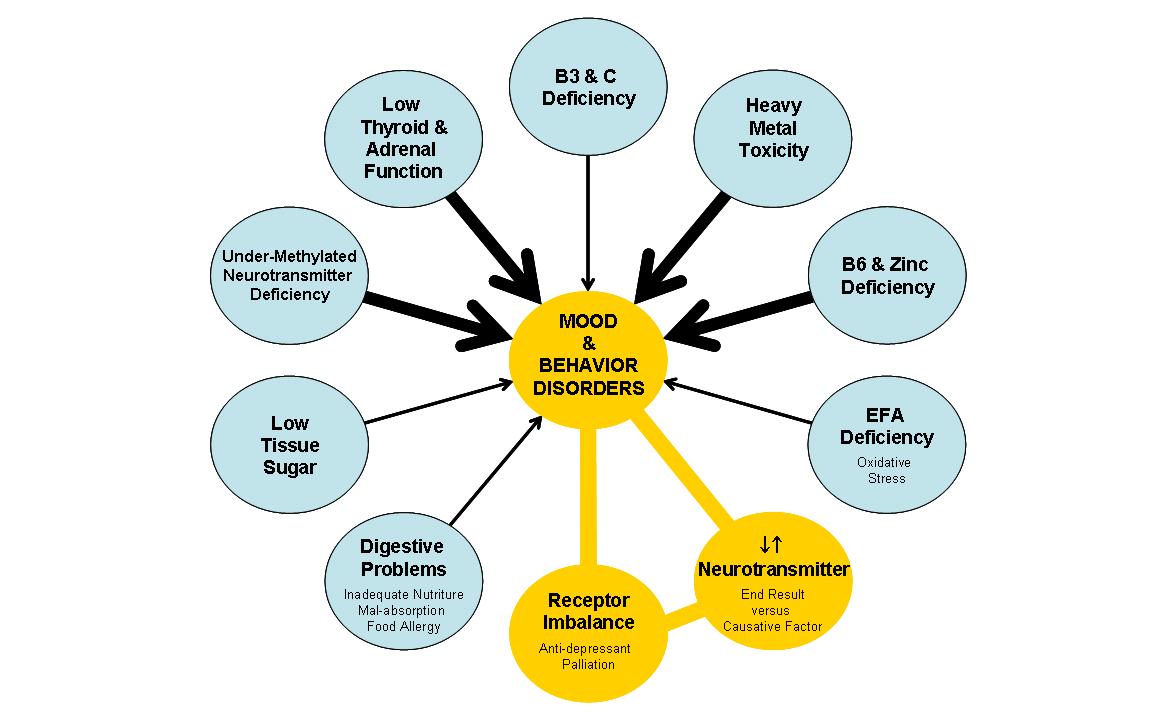
Figure 1 is a schematic of the key causative factors of mood and behavior disorders. Modern research continually confirms that these factors are important in mood and behavior disorder pathophysiology. The list of assessments and treatments described herein are not exhaustive but represent the core considerations for optimal complementary treatments for kids with mood and behavior disorders. Orthomolecular treatment can be implemented safely as an adjunct to conventional psychiatric therapy.
Figure 1. Mood and Behavior Disorders: Summary of Causative Factors
Kid specific aspects of orthomolecular treatment will be the focus of this series. Mood and behavior conditions that we are looking at include anxiety, severe depression, bipolar disorder, hormonal depression, other endogenous depressions (cyclothymia, seasonal affective disorder), OCD, ADHD, ODD and, addictive behavior. Kids emerging from their early teens sometimes face early onset psychosis so we have dedicated an orthomolecular treatment article on this topic as well. Kids with autism spectrum can benefit from orthomolecular treatment and although this series does not cover that subject, families are encouraged to examine the International Schizophrenia Foundation archive and referral network.
Biochemical syndromes of importance for kids with mood and behavior disorders are those that ultimately influence neurotransmitter production, release, inhibition, and signal transduction.1
Various segments of the mood and behavior disorder population of kids fall into subgroups of distinct biochemical imbalance. We often see subgroups of essential fatty acid deficiency, inadequate nutriture (protein deficiency), dysglycemia, food sensitivity, digestive compromise, mal-absorption, under-methylation, vitamin B3 deficiency & vitamin C deficiency, heavy metal toxicity, B6 deficiency, zinc deficiency, magnesium deficiency, calcium deficiency, and hypothyroid and hypoadrenal states. The goal of orthomolecular medicine is to attempt to correct the causative factors of these biochemical imbalances, rather than letting them worsen and dominate metabolism.
Kids with mood and behavior disorders have similar nutritional imbalances to adults and there is often an overlapping of symptoms and diagnoses.
Anxiety, for example, often coexists with depression. Depression often involves negative thought rumination and sadness. Stoic depressive kids rarely smile and are locked in despair sometimes with suicidal thoughts. Suicidal propensity is global in patients with depression, anxiety and behavior disorders. Obsessive thinking is commonly found in anxiety disorder cases but, is not diagnostic for obsessive compulsive disorder (OCD) unless it is so severe that it profoundly interferes with thinking and behavior. Kids with addictive behavior often have co-existing mood dysfunction, behavior disorders, or sometimes schizophrenia. Addictive behavior ranges from the realm of illicit substance use and alcoholism to compulsive behaviors and gaming addictions. Kids with anxiety are over-stimulated and in advanced stages this is disruptive. Anxiety can be associated with phobic disorders and in some cases schizophrenia. Over-stimulated states of anxiety are typically uncomfortable and not productive (i.e. your performance level is diminished). Conversely, in bipolar/manic depression, over-stimulated states (mania) can often be productive with reports of accomplishing tasks with immense intensity and creativity. In bipolar disorder, mood often cycles to a deep depressive burn out phase. In depression and anxiety we often see inattention which can be mild or, in severe cases, interfere with thought processing. In children and adults, advanced inattention can be seen as a pure component of ADHD. Inattention can be due to ‘thought blocking’ which is an interruption in the processing of thoughts for short periods of time; thought blocking is commonly seen in kids with heavy metal excess. Irritability is found globally in all mental illness; anger and irritability are often linked to the ‘stuckedness’ of depression or hypoglycemic (low blood sugar) tendencies. Anger can extend into the realm of criminal behavior.
Neurotransmitter deficient syndromes in kids with mood and behavior disorders
Depression is used here as a classic example of a neurotransmitter deficiency syndrome. Based on current research, mixed neurotransmitter theory states that depression is caused by reduced numbers of brain neurotransmitters. Serotonin and the catecholamines are the brain’s master neurotransmitter systems. The catecholamines include dopamine, norepinephrine, and epinephrine. Conventional drugs (re-uptake inhibitors; SSRI’s, NRI’s, or SNRI’s) attempt to increase synaptic availability of one or both of these master neurotransmitter pathways. These drugs depend on brain cells having enough neurotransmitter to do the job.1 In clinical settings we see many kids on medications that either are not working or have been working less effectively with increased use and, in such cases, there is often an increase in dosage, medication change or, another medication is added. Conventional re-uptake inhibitors increase the synaptic concentration of neurotransmitter (by keeping neurotransmitters in the synaptic cleft) but do not act to increase the total number of neurotransmitters made which is unfortunate because the brain’s natural response is then to down-regulate the natural production of the neurotransmitter pathway targeted by the medication (down-regulation is a normal homeostatic process mediated by MAO and COMT). The end result is a further depletion of already low neurotransmitter levels. Many kids with mood and behavior disorder can be caught up in this type neurotransmitter deficiency state.
Part Two of this series will cover Under-Methylated Kids and Kids with Heavy Metals.
References
1. Delgado PL, Moreno, FA: Role of norepinephrine in depression. J Clin Psychiatry. 2000; 61(Suppl 1): 5-12.
MindCheck is the Weekly Wednesday Kids Mental Health series with Dr. Ray Pataracchia, N.D. MindCheck provides in depth information on the orthomolecular approach to coping with mood and/or behavior disorders. The MindCheck Health Series is endorsed by the Mindful Network – ‘A Better Future for Children’s Mental Health’.